How To Find the TCN in MedBatch
The TCN is the Transaction Control Number. This number is assigned to a claim when it is submitted and is used by eMedNY to identify individual claims.
Payer Claim Control #
Method 1
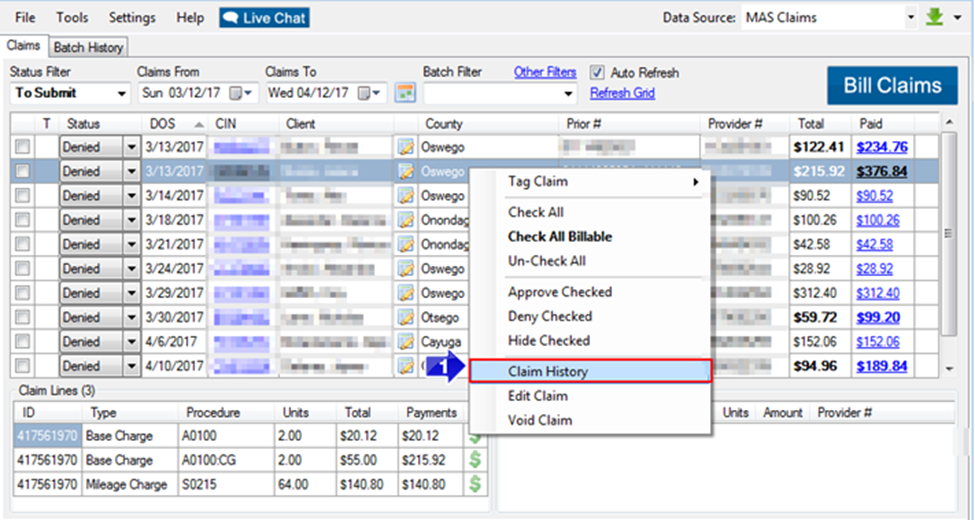
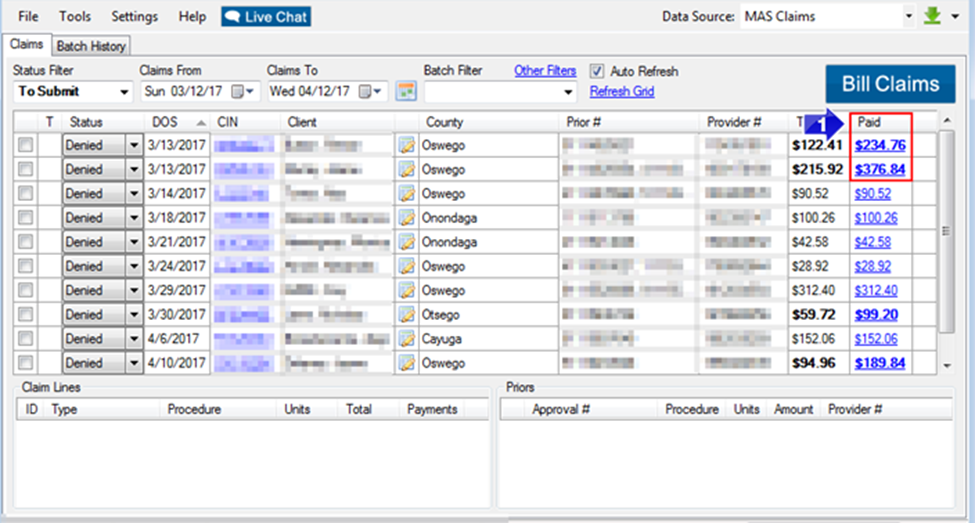 1. If the claim has received a full or partial payment, the TCN can be found by clicking on the paid amount in the claims grid.
1. If the claim has received a full or partial payment, the TCN can be found by clicking on the paid amount in the claims grid.

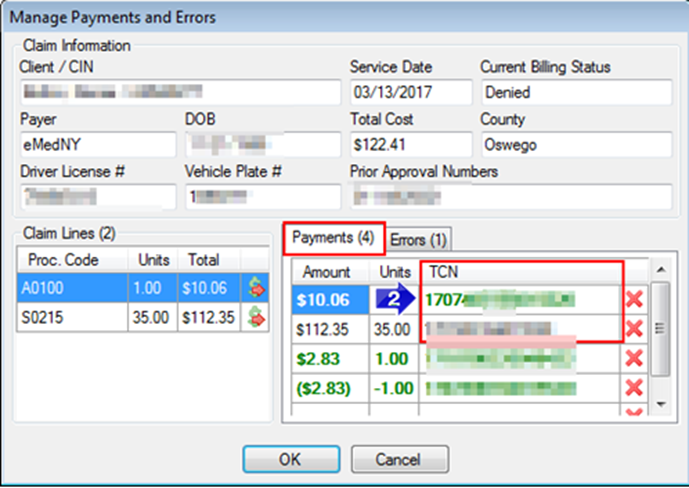
2. The Manage Payments and Errors window will open. Notice the TCN found under the Payments field.
Method 2

1. If the claim hasn’t received any payment, there will not be a TCN in the Payment Right click on the claim and select Claim History to open the Claim History window.

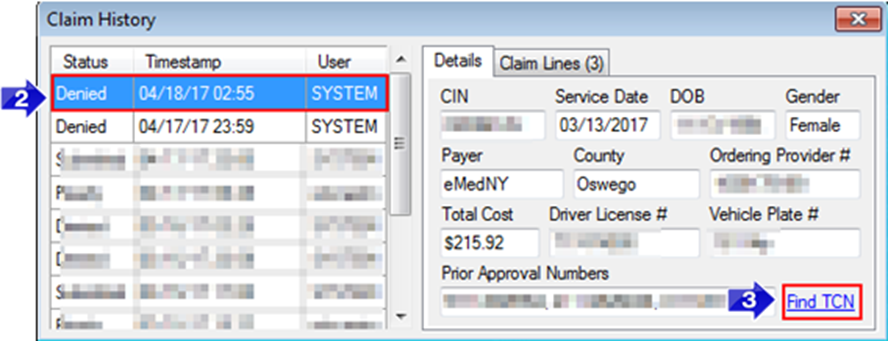
1. Select the latest Status provided by eMedNY.
2. Click Find TCN.

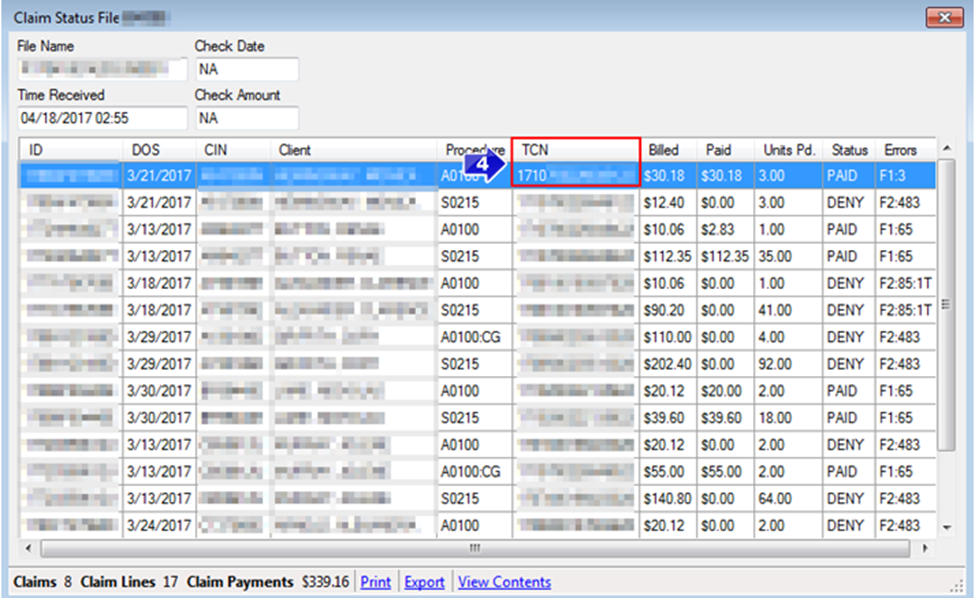
4. This will take you to the Claim Status File The TCN will be highlighted.
![New Founders Software-White.png]](https://help.intelligentbits.com/hs-fs/hubfs/New%20Founders%20Software-White.png?height=50&name=New%20Founders%20Software-White.png)